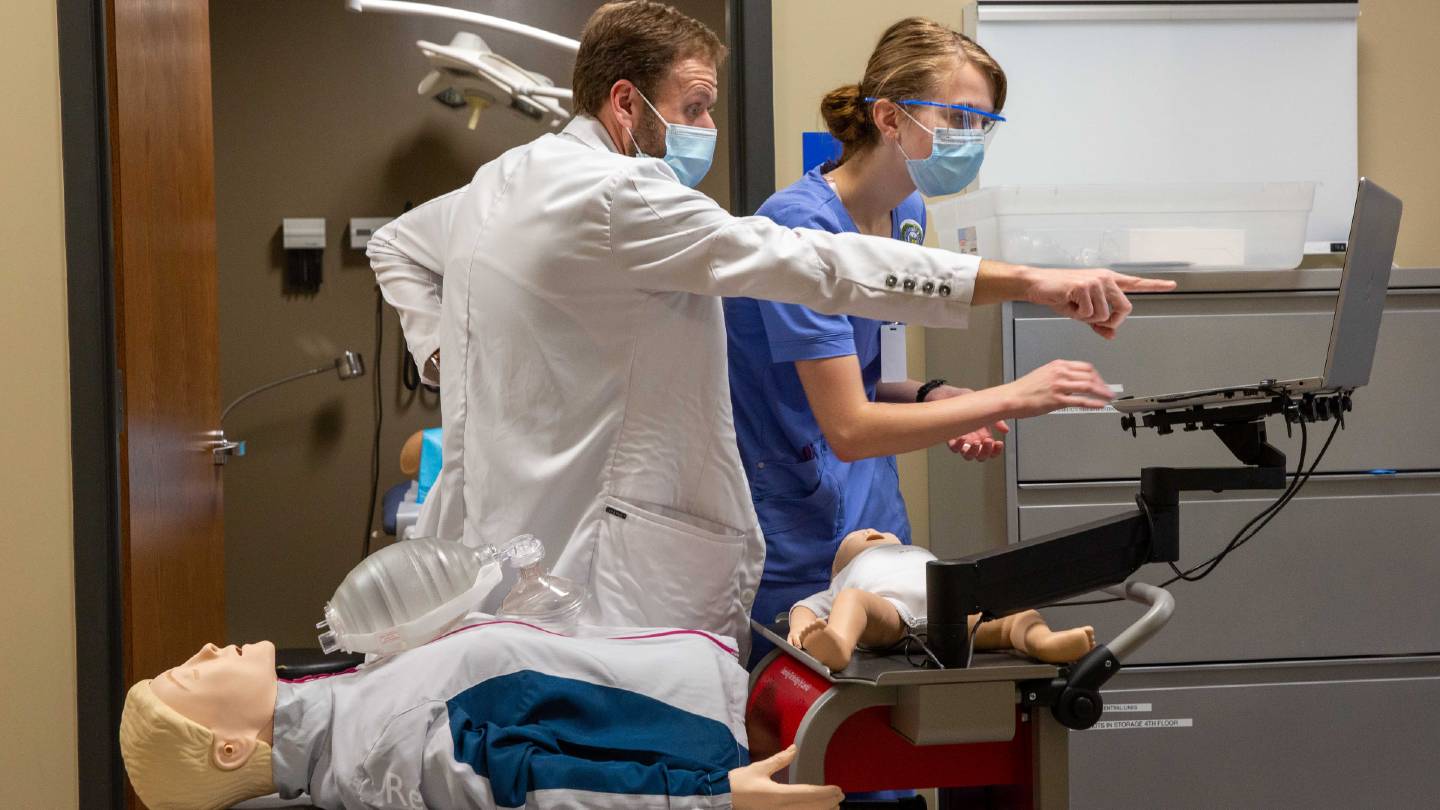
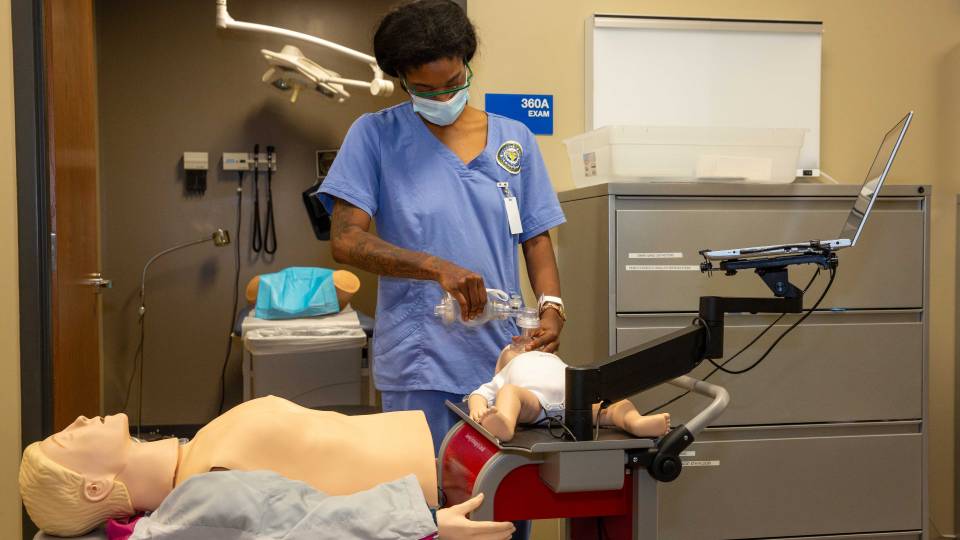
Dr. Joseph Chamness guides first year UAH College of Nursing student to become certified using new CPR skills station.
The University of Alabama in Huntsville (UAH), a part of The University of Alabama System, announced that the UAH College of Nursing has been selected by the National League of Nursing (NLN) as one of only 12 nursing programs across the U.S. to become early adopters of a new CPR training program called Resuscitation Quality Improvement (RQI).
The UAH CON will work as an NLN Change Agent in collaboration with the NLN, Laerdal Medical and RQI Partners to pioneer a new method of CPR training that will prepare future nurses to enter the healthcare field with an enhanced means of teaching high-quality CPR. Implementing this advanced training is thought to dramatically improve patient outcomes and save many more lives.
With this selection, UAH Nursing joins an exclusive group of RQI early adopters that will provide valuable insight into the development of an innovative solution specifically tailored to the more than 150,000 students who graduate annually from nursing and allied health education programs at U.S. colleges and universities.
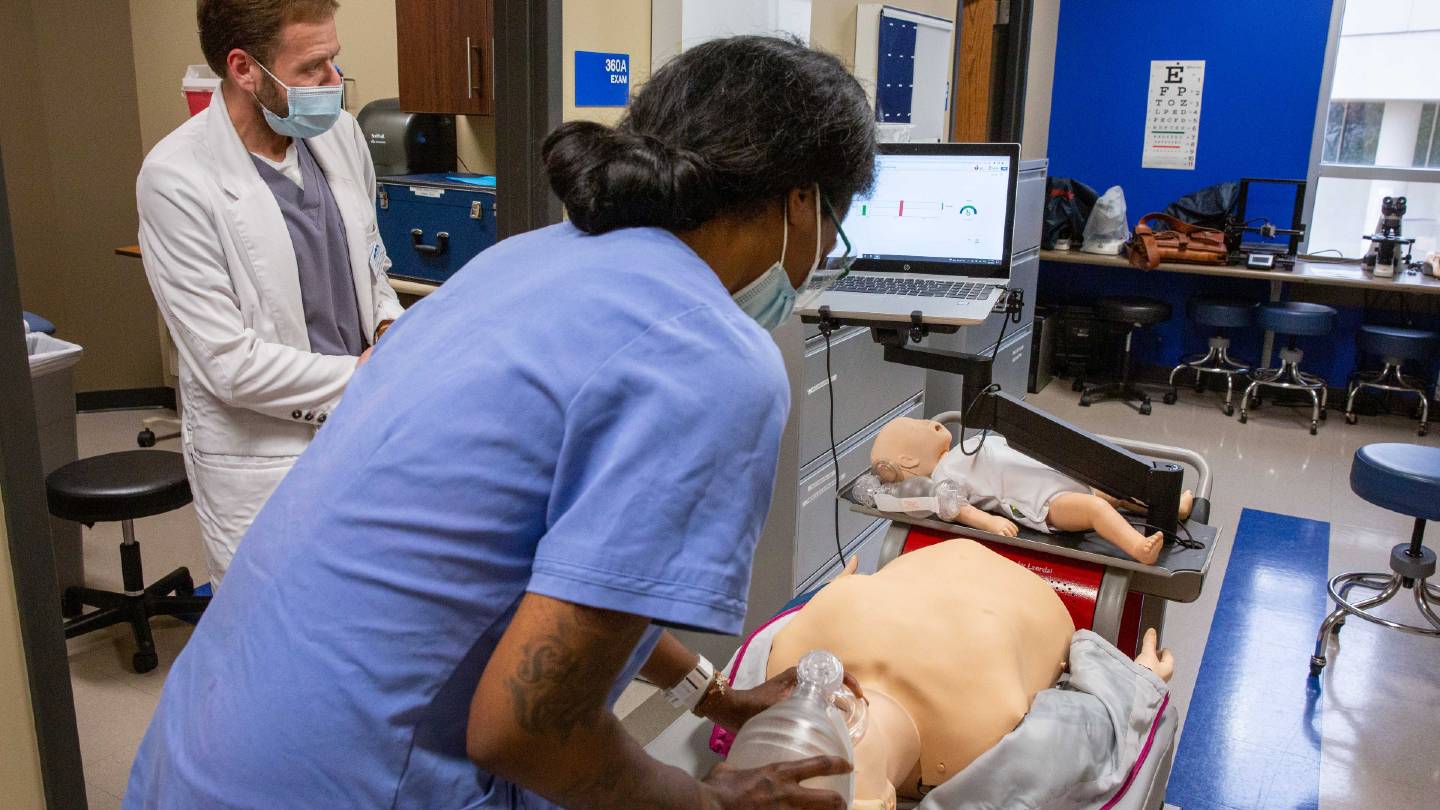
CPR certification is required before students enter the UAH nursing program. The current model is that there is a revalidation every two years, a pattern that has been established ever since CPR was initiated for any health care professional.
“RQI is new in nursing education,” says Dr. Karen Frith, dean of the College of Nursing. RQI offers a new method of refresher training that follows a more frequent schedule to keep CPR skills sharp.
“Many of us know that if you don’t do something more than once every two years, that your skills decay,” explains Dr. Frith. “So, with RQI, every three months students go through a short burst of education online, and there is a skills component follow-up as well.”
Anyone who has ever taken a course in CPR is familiar with the traditional training method, which is performed with a static mannikin, whether an adult, infant or child model, and an instructor who observes the participant in action and guides them in the proper way to best perform CPR. RQI is an innovation that reinvents the way students are trained, using the latest technological advances to improve the process.
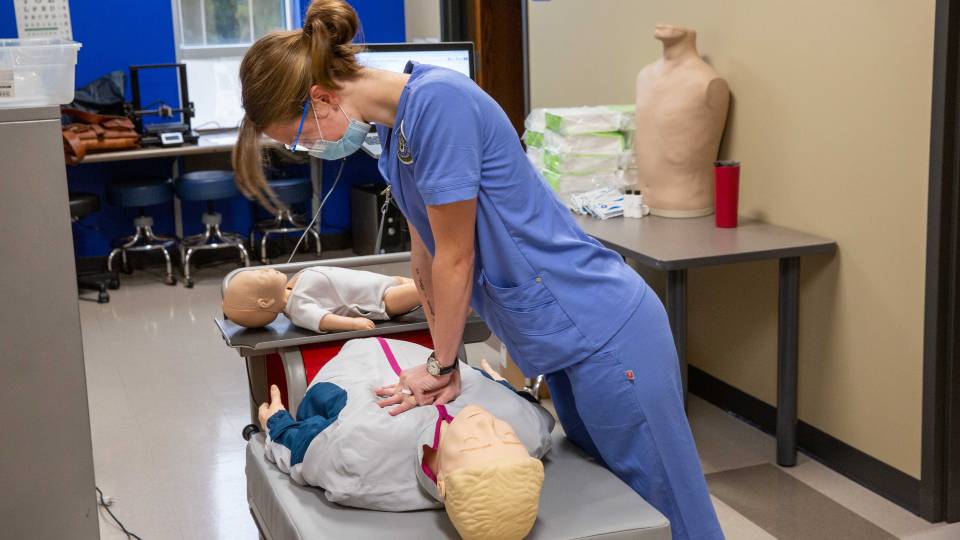
“We have a CPR cart with a mannikin and a computer, and Artificial Intelligence (AI) is built into the CPR software,” Dr. Frith says. “While the person is revalidating their CPR skills, if they are not compressing the chest fast enough or deep enough on the mannikin, for example, the AI will say ‘increase the depth’ or ‘increase the rate.’ So the students are getting real-time feedback about how effective their skills are.”
With the help of AI, the CPR student receives tailored feedback that is not really possible otherwise, even with the help of an experienced instructor.
“The compression depth and rate are the most important parts of CPR,” says Dr. Frith. “The traditional instructor is knowledgeable, and they go through additional training, but they still don’t have the standardized assessment for things like the depth of compression. You can’t know that by visual means alone. This AI-backed machine is able to give better feedback to the student. Also, when they do it every three months, those skills don’t decay. This is a real change in what nursing schools will do, to adopt this model.”
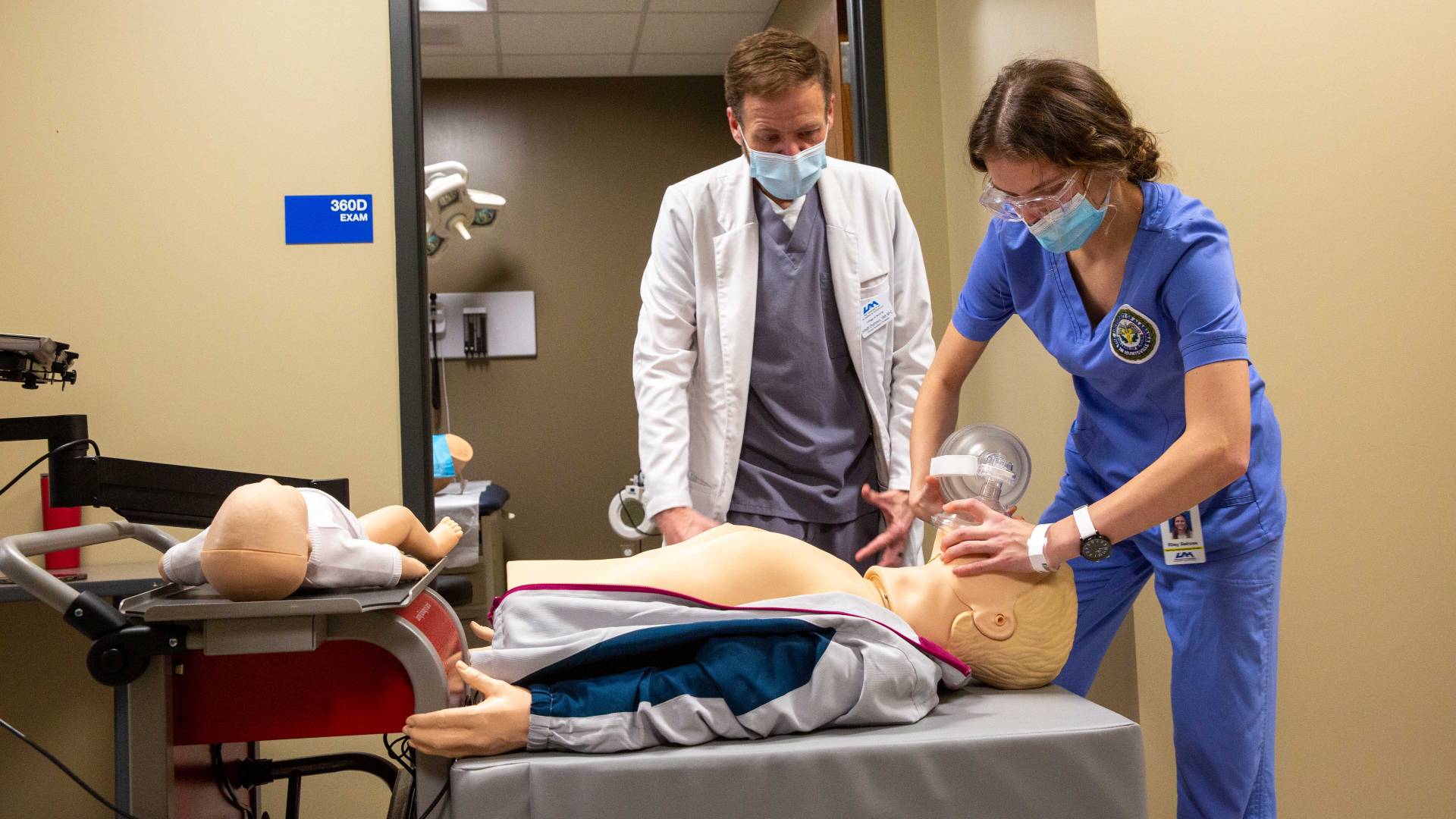
The new process is based on research studies that have been done by nurse educators who found that small-dose CPR revalidation keeps the knowledge fresh in the student’s mind.
“What we’re doing is testing how to roll this out as an education program and giving feedback to the NLN about how we would suggest other schools will do it,” notes Dr. Frith. “We had a zoom interview with them, and they assessed our readiness and our commitment to becoming a Change Agent of CPR education.”
Every year, 475,000 people die from cardiac arrest in the United States, and more than 200,000 cardiac arrests occur in U.S. hospitals. In the U.S., only 25% of patients survive an in-hospital cardiac arrest; just 10% survive out-of-hospital emergencies. High-quality CPR is the single highest determinant of survival from cardiac arrest. The ability to consistently administer high-quality CPR is critical to improving outcomes and is considered the last chance for survival in a cardiac arrest emergency.
“This is about the effectiveness of the CPR. If the person doing the CPR is not as effective as they need to be, the brain doesn’t get as much oxygen through manual compression. That lack of effective CPR is a problem,” notes Dr. Frith. “They might have some brain damage, some organ damage, kidney failure. The brain is the most sensitive. That results in a stroke, lack of oxygen and damage to the brain.”
With the help of Change Agents like the UAH CON, RQI could ultimately become the new standard for this kind of care. RQI students use low-dose, high-frequency quality improvement sessions to measure and verify competence.
“What this is, is short education,” says Dr. Frith. “The first time the student does the training it takes about 45 minutes to an hour to go through the online part. The in-person interacting is around 15 minutes, and it is still much more effective than doing four to eight hours every two years.”
Dr. Joseph Chamness, a clinical assistant in the CON and the administrator of the program, has extensive experience in emergency rooms and as a Nurse Practitioner.
“With all my years in critical care, I was very excited to take on the opportunity to implement this program,” Dr. Chamness says. “Drs. Marilyn Oermann and Suzan Kardong-Edgren conducted numerous studies that have shown CPR skills are lost due to only performing CPR once every two years. Many nurses even working in a hospital can go months to years without ever performing any CPR, except for their recertification classes. The RQI program that has been implemented in hospitals already across the nation has seen an improvement of survival skills by up to almost 50%.”
One of the primary benefits of the new program “is that it runs itself without requiring someone specially trained to teach CPR,” Dr. Chamness says. “The program also is able to get more students trained in a shorter amount of time. It can measure the depth of compressions, full recoil of the chest, rate of ventilations and volume of air delivered with ventilation compared to what a teacher can do by just watching and guessing that all of these aspects are correctly done. We currently have 56 students enrolled in the program. It has been a huge honor to be a part of this change to improve CPR education.”
Dr. Frith relishes being a part of this change as well.
“It takes about 15-20 years for research that has been initiated to change a practice. That’s why this is so important, the active research to push that change forward. The reason we wanted to be a part of this is the potential for our students to save more lives. And we want to always be leading change and leading innovation in healthcare.”
Contact
Dr. Joseph Chamness
256.824.2470
joseph.chamness@uah.edu
Jane Armitage
256.824.6345
jane.armitage@uah.edu
Russ Nelson
256.824.2101
russell.nelson@uah.edu
